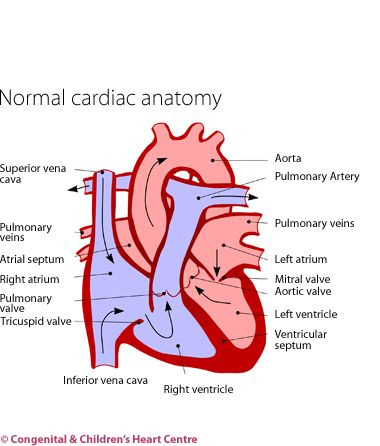
Dilated Cardiomyopathy in Childhood
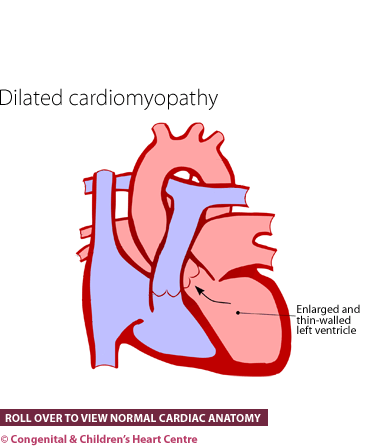
What is it?
Dilated cardiomyopathy is a serious condition in which the heart muscle is weak and incapable of pumping as much blood as it should.
The blood waiting to get into the heart develops a high pressure and this can cause fluid to leak out of the blood vessels into the lung (pulmonary oedema). The amount of blood that the heart can pump is severely reduced and this is even more of a problem on exercising.
What causes it?
Dilated cardiomyopathy has many causes, not all of which are known. In some infants and children, it has been present since birth and even before, though undetected. The cause may be defective heart muscle, a problem with the way in which the heart uses nutrients (a metabolic cause) or a syndrome. These, in turn, may be due to a genetic problem and can run in a family.
In another group of infants and children, dilated cardiomyopathy occurs as a consequence of a viral infection such as coxsackie. This can cause an inflammation of the heart known as acute (sudden) myocarditis. When the inflammation settles, heart function may slowly return to normal but, in some people, it persists and is then indistinguishable from dilated cardiomyopathy. These viral infections can even occur in the womb and, if the damage does not resolve itself, the infant may be born with dilated cardiomyopathy. In many cases, a cause is never found.
How many people get it?
The prevalence of all types of cardiomyopathy has been estimated as approximately one case every year out of every 100,000 children younger than 10 years of age.
Who gets it?
Anyone can get dilated cardiomyopathy. It can occur at all ages – from fetal life through childhood to old age. In children, it is most common in infants (less than one year old).
What are the signs and symptoms?
Both dilated cardiomyopathy and inflammation of the heart (acute myocarditis) present in similar ways and it is often impossible to distinguish them without performing tests. Often the condition starts with symptoms of a viral respiratory infection with:
- breathlessness
- difficulty feeding
- sweaty on feeding
- vomiting
- lethargy
- diarrhoea
- muscle pains
- sudden collapse
- general malaise in older children
With the advent of fetal echocardiography, the diagnosis of dilated cardiomyopathy can be made in the womb.
What kind of tests might I have?
Children are referred to a paediatric cardiologist, who will investigate further. After questioning the parents to obtain the child's history and examining the child, several tests will be organised. These will usually comprise an electrocardiogram (ECG) to measure the electrical activity of the heart and a chest X-ray to visualise the heart and lungs. The diagnosis is made by echocardiography. Some blood and urine tests may also be necessary to attempt to find a cause.
In the long term, repeated echocardiograms will be performed to assess the cardiac function and assess recovery.
What is the treatment?
In mild cases:
- Diuretics to encourage the child to pass urine and reduce the water retention
- ACE inhibitors such as captopril, enalapril or lisinopril to make the work of the heart easier
- Beta blockers such as carvedilol may be used to slow the filling of the heart
- Digoxin may be used in addition to the above.
In severe cases:
- Ventilation on an intensive care unit
- Drugs to stimulate the heart (known as inotropes), such as adrenaline
- Heart transplantation
If the condition is suspected to be acute myocarditis, immunoglobulins may be used.
Are there any complications of the condition?
Many infants and children with mild cardiomyopathy suffer no complications. In severe cases there can be major complications to vital organ systems and even death.
What is the prognosis?
Of those who are taken to their doctor with severe heart failure, approximately one third make a complete recovery, one third recover but remain on medicine to assist heart function and one third either die or require a heart transplant. Outpatient visits may be lifelong, with repeated echocardiograms to assess cardiac function.
When the heart function is very poor and does not recover, a heart transplant may be considered.
Download Dilated Cardiomyopathy in childhood PDF![]()
Further information at
The Children's Heart Federation and The Cardiomyopathy Association