Hypertrophic Cardiomyopathy in Childhood
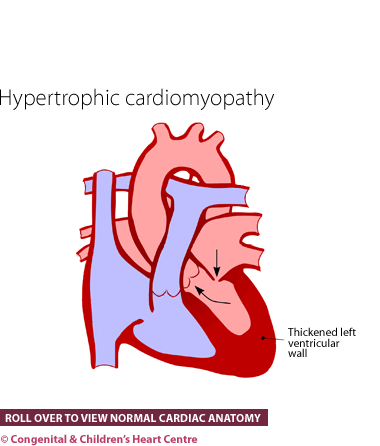
What is it?
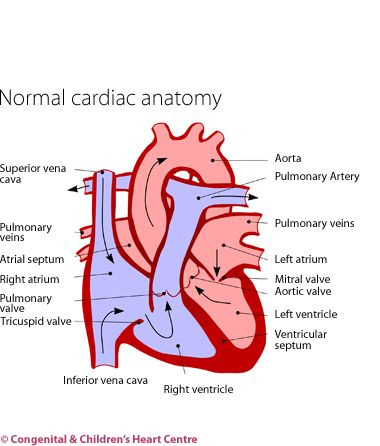
Hypertrophic cardiomyopathy is a serious condition in which the heart muscle is thickened which may lead to problems with the rhythm and function of the heart.
What causes it?
Hypertrophic cardiomyopathy has many causes, not all of which are known. In some infants and children, it has been present since birth and even before, though undetected. The cause may be defective heart muscle or a problem with the way in which the heart uses nutrients (a metabolic cause) or a syndrome. These, in turn, may be due to a genetic problem and can run in a family. In many cases, a cause is never found.
How many people get it?
The prevalence of all types of cardiomyopathy has been estimated at approximately one case every year out of every 100,000 children younger than 10 years of age.
Who gets it?
Anyone can have hypertrophic cardiomyopathy. It can occur at all ages – from fetal life through childhood to old age. Conditions such as Noonan's syndrome are associated with the disease. It tends to run in families but often it may be a new occurrence.
What are the signs and symptoms?
Often there are no symptoms and the disease comes to attention due to the presence of a murmur (extra sound in the heart), or as a result of screening where a close family relative has the disease. Infants may present with breathlessness on crying or feeding. Children and teenagers may present with palpitations or sudden collapse on activity.
With the advent of fetal echocardiography, the diagnosis of hypertrophic cardiomyopathy can be made in the womb.
What kind of tests might I have?
Children are referred to a paediatric cardiologist, who will investigate further. After questioning the parents to obtain the child's history and examining the child, several tests will be organised. These will usually comprise an electrocardiogram (ECG) to measure the electrical activity of the heart and a chest X-ray to visualise the heart and lungs. The diagnosis is made by echocardiography. Some blood and urine tests may also be necessary to attempt to find a cause.
In the long term, repeated echocardiograms will be performed to assess possible progression and heart function. Twenty-four hour ECG monitoring, event monitoring and exercise stress testing will be necessary to detect rhythm disturbances of the heart. An MRI may provide useful information.
What is the treatment?
There is no cure for most types of the disease and treatment involves minimising the risk of complications.
In mild cases:
- Observation alone may be needed.
- Beta-blocker medication to reduce the contractility of the heart
In more severe cases:
- Additional medicines may be needed such as anti-arrhythmics to stabilise normal heart rhythm
- Surgical debulking of the thickened muscle under the aortic valve
- Implantable defibrillator
- Transplantation
Are there any complications of the condition?
Many infants and children with mild hypertrophy cardiomyopathy may suffer no complications throughout their whole life. In other cases the disease can progress and lead to complications such as chest pain (angina), syncope (fainting), heart rhythm disturbances and even fatal cardiac arrest.
What is the prognosis?
This is highly variable depending on the underlying cause. Family history is often a good guide to outcome. Outpatient visits may be lifelong, with repeated echocardiograms to assess cardiac structure and function. In some cases heart transplantation is required although this is in only a small proportion.
It is important that such children are cared for by doctors experienced in treating such conditions.
Download Hypertrophic Cardiomyopathy in childhood PDF![]()
Further information at
The Children's Heart Federation and The Cardiomyopathy Association